Takeaway
The Issue
St. David’s Foundation fosters innovation and supports services that help older adults live safely and independently. We believe that as we age, it is important for older adults and their families to plan for care at the end-of-life. Ultimately, we want to ensure that end-of-life care is of high-quality and in accordance with one’s wishes. End-of-life planning can be a challenging and uncomfortable topic, but there is widespread recognition of its critical importance in ensuring better end-of-life experiences. By having early conversations, individuals and their loved ones can be more prepared for the difficult decisions that will affect us all at some point.
Considering these issues, St. David’s Foundation commissioned PerryUndem, a national research firm, to conduct a statewide survey to explore the attitudes, experiences, and needs of Texans regarding serious illness and end-of-life issues. This statewide survey compares the expectations and realities of end-of-life care and planning.
The Findings
Most Texans have similar preferences at the end of their lives – such as wanting to die at home, being able to afford care, and not burdening their loved ones. Despite shared preferences, just 37% of Texans said their loved one’s end-of-life went the way they wanted it to go. Hospice care, location of death, and insurance status were associated with more positive end-of-life experiences. The research found disparities in access to end-of-life care with Black and Latino respondents and more barriers to accessing the care they needed.
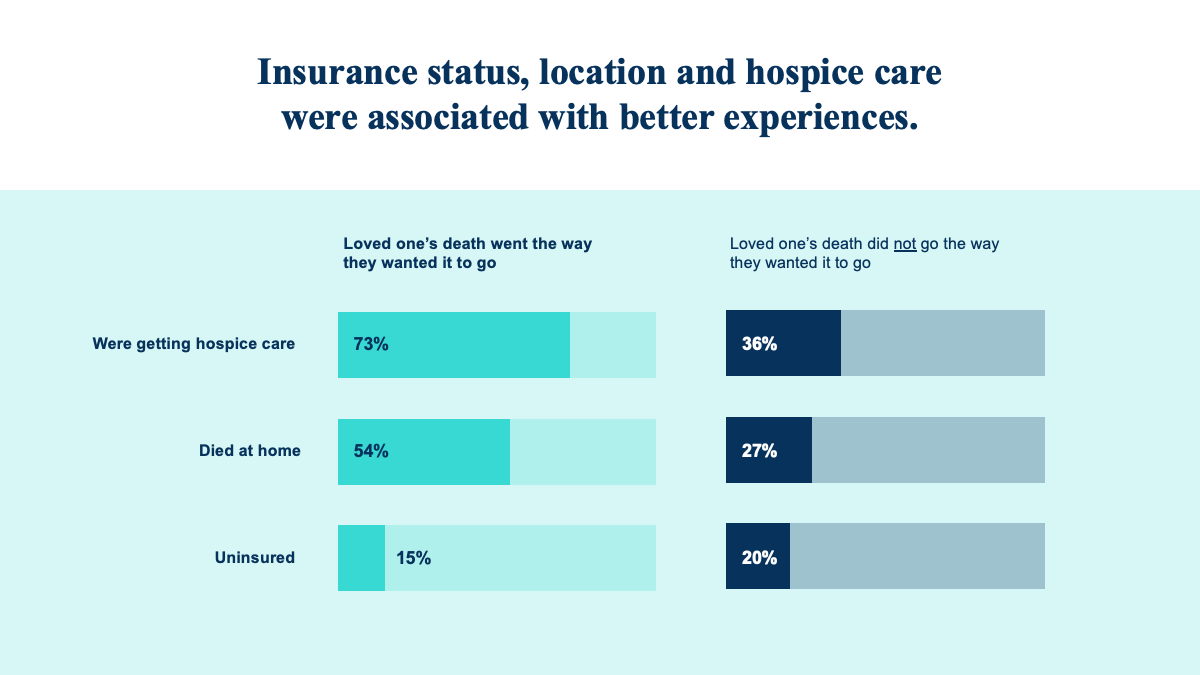
Most Texans, even older adults, are unprepared for decisions about end-of-life care. The vast majority believe it is important to have their wishes in writing, yet over half have not done so. Similarly, many say they would like to discuss end-of-life planning with their health care provider if they were faced with a serious illness, yet only 17% have had a provider initiate a conversation about it.
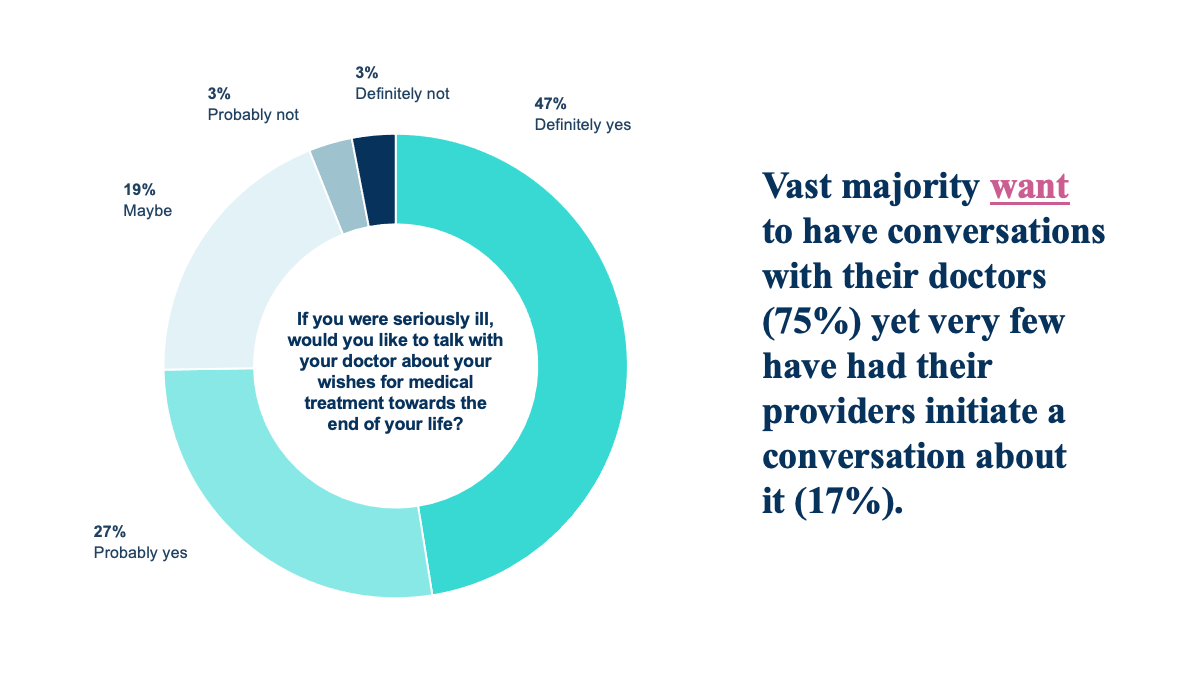
Gaps in preparation are tied to trust in the healthcare system, highlighting the importance of addressing underlying systems alongside efforts focused on individual preparation.
The Foundation’s goal is for these findings to equip Texans with information and data to increase awareness around end-of-life resources and advocate for systemic improvements to support all Central Texans in having a positive end-of-life experience.
If you are interested in full presentation materials and companion notes or would like to schedule a presentation of the research findings, please contact [email protected].
Read more: Study Finds Gap Between What Rural Residents Want for End-of-Life Care and What They Receive
Recommended Reading
-
Story
October 18, 2021
-

